Cost of homeless care increases

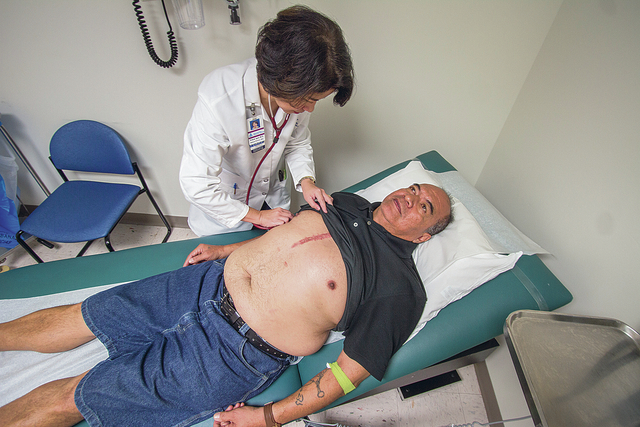
DENNIS ODA / DODA@STARADVERTISER.COM
Hospitals are incurring costs to care for homeless patients, many of whom have chronic illnesses. Last month Dr. Fritzie Igno of Queen Emma Clinics checked Alexander Akuna, a former homeless patient whose heart and kidneys were failing. He now lives in federally subsidized housing and says he is surviving what doctors told him were terminal illnesses.


Alexander Akuna was living on Nanakuli beach in 2009 when his heart and kidneys began to fail.
The 57-year-old was in and out of the Queen’s Medical Center over the next year for multiple chronic diseases brought on by drug use, poor nutrition and living in harsh conditions.
“It would be no longer than three days and I’d be back,” Akuna said. “I stayed in the hospital more than I went back home.”
Akuna is one of thousands of homeless patients who frequent Hawaii hospitals, many of whom have chronic health conditions that often lead to costly emergency room visits and repeat admissions. He ended up in the hospital for a year and a half, which, for a typical patient with significant health care needs, can cost as much as $1 million.
The costs are absorbed by the facility, privately insured patients and taxpayers. With homelessness on the rise, hospital visits and medical costs are rapidly climbing.
“The problem is not declining. It is increasing, and the community and community organizations like Queen’s are having to bear the responsibility,” said Art Ushijima, Queen’s president and CEO.
Don't miss out on what's happening!
Stay in touch with breaking news, as it happens, conveniently in your email inbox. It's FREE!
Queen’s cared for homeless patients 10,126 times in 2015, resulting in gross charges of $89.3 million, according to research by the Hawaii Health Information Corp. That’s up from 9,301 patients and gross charges of about $80 million in 2014 and 6,958 patients and $54.8 million in 2013. Queen’s is on track to see an estimated 10,459 homeless visits this year with total gross charges of $100.2 million.
Gross charges are the total billed to a patient and are often substantially higher than what is covered by health insurance. Patients might or might not have to pay the balance, depending on a hospital’s billing agreement with insurers.
Medicare and Medicaid, the government health insurance programs for seniors and low-income residents, pick up some of the cost of homeless care. But Queen’s calculates it absorbs about $5 million in unpaid homeless expenses each year.
Akuna said he has turned his life around after 27 years of drug use and crime, and is surviving what doctors told him were terminal illnesses. He now lives in federally subsidized housing and is looking for a job.
“After all that time in and out of the hospital, you have to make a change for yourself. I give all the glory to God. It really took a miracle for save me,” he said.
Statewide, hospitals treated homeless patients 15,900 times last year, up from roughly 14,900 times in 2014, HHIC data show.
“For the most part, emergency rooms in the 21st century have replaced the churches of old,” said Dr. Daniel Cheng, assistant chief of Queen’s emergency department. “We’re talking about medical care, shelter and basic human decencies like food, clothing.”
Many in the homeless population come into the ER with multiple medical conditions when the problem has become acute and they need high-level care, he said.
“It’s the same medical conditions that you and I get times 10 because of the severity,” Cheng said.
Hawaii Pacific Health, parent company of Kapiolani Medical Center for Women &Children, Pali Momi Medical Center, Straub Clinic &Hospital and Wilcox Medical Center on Kauai, said that in the last year it has seen a 20 percent spike in the high-risk population, many of whom are homeless and typically stay in the hospital more than two days longer than other patients, largely due to a lack of appropriate post-acute care facilities.
“They’re the sicker population,” said Judy Suzuki, head of the hospital case management and medical social work department at Straub Clinic &Hospital. “They (often) have mental illness, substance abuse and a history of incarceration. After they’re medically stable … they need continuing skilled care. There really isn’t an appropriate setting for this population; that’s why hospitals are struggling with that.”
Hawaii Pacific Health has had to negotiate to have nursing homes and rehab facilities take homeless patients, often by agreeing to pay for short-term stays at a YMCA, hotel or respite home for days or a week during recovery, said Suzuki. Straub has spent between $30,000 and $50,000 in the last year to house the homeless after their hospital stay.
“The majority of them either need IV antibiotics or wound-care management or short-term rehab,” she said. “If they have addiction or behavioral problems, an appropriate post-acute facility is almost nonexistent. So a lot of times they end up sitting here in acute-care beds.”
Adding to the cost of homeless care is that in many cases they are brought to the hospital by ambulance, which costs about $1,000 per transport.
The City and County of Honolulu’s Emergency Medical Services has been overwhelmed with the increasing number of calls for homeless.
One EMS worker estimated that paramedics sometimes transport 12 homeless people to the hospital in 12 hours, often for minor ailments, prescription refills and food, which do not warrant use of ambulance services.
On some days the number of 911 calls for homeless can average 50 percent to 70 percent of all calls, based on anecdotal evidence, the EMS worker said.
“We have an epidemic of over-utilization of EMS service by the homeless. The only people it hurts is people with true life-threatening emergencies and there is no ambulance to take care of them,” said the EMS employee, who asked not to be further identified because he wasn’t authorized to speak to the media. “It is a huge problem. I don’t think people understand the seriousness of over-utilization.”
Five of the top 10 repeat 911 callers were homeless from January through May, according to EMS. The top homeless patient has called the ambulance 157 times this year.
“EMS is very familiar with the homeless patients who call us on a regular basis, and we do know them by name,” said EMS Chief Dean Nakano. “EMS supports working collaboratively with the hospitals and social service partners in an effort to address the needs of the homeless community, whether that be community paramedicine or a similar service.”
A community paramedic program intended to reduce overuse of ambulances by chronic 911 callers was shelved in 2013 due to a lack of resources. The program would have established two community paramedics who would have visited the top 50 callers and directed them to more appropriate care. Similar programs nationally have been shown to decrease the number of unnecessary 911 calls.
Queen’s has started a program to identify the top 25 repeat visitors, or “hyper users,” to get control over the expanding unpaid homeless bill by providing preventive services and follow-up care outside the hospital. The top 25 repeat visitors came to Queen’s an estimated 1,514 times. Gross billings for both hospital and physician costs totaled roughly $12 million.
“Like many illnesses, you really need to deal with it through preventive services,” Ushijima said. “You have to deal with it on the front end. That means getting into housing, good nutrition, having jobs and providing them a source of income. Those kinds of things can mitigate the demand for medical services. We want to be contributing solutions to this problem before it becomes so overwhelming that we can’t deal with it.”
21 responses to “Cost of homeless care increases”
Leave a Reply
You must be logged in to post a comment.




Instead of going to private hospitals, the homeless should be going to a public clinic operated by the state with federal backing. This is one reason why your health insurance is sky high, you’re paying for the uninsured.
YUP. Sad how we pay for other people’s BAD choices in life.
Sadder yet is that under our laws pest-like people cannot be eliminated.
You’ve recognized the same thing that I saw. In most large cities and states there are government hospitals that care of the indigent. In Hawaii/Honolulu there are virtually no public facilities. It seems by design our local governments have decided to dump this problem on the private sector. That’s what happens when our legislature cares more about funding the unions than they do about the welfare of the average citizen.
True statement.
What the heck are they doing with phones in the first place ? Sometimes you have to give them tough love to make them understand what they are doing is wrong. This is blatant abuse of services and should be treated as a criminal matter. Maybe a thirty, sixty or 90 day jail stay would get their mind right.
You mean it took him 27 years to finally grow-up?? He made those choices not any of honest tax payers who’s rising medical care cost us more because of his own actions. Why should I pay for his bad choices?????
Fully agree!!!!
Agree!
Other countries laugh at the US. They say the US is the only country with fat poor people. Now they have another reason to laugh while we cry with our wallets.
Using an acute care facility to treat individuals with long term chronic illnesses is costly and inefficient. These individuals need to be on Social Security/SSI and Medicare/Medicaid. Perhaps a combined Social Security Administration / Dept. of Human Servuces outreach effort can help get the financial/medical foundation established for individuals with chronic long term illnesses. Yes, it can take some time for a decision, but State of Hawaii could legislate an interim payment program. Once finances and medical coverage are in order, social workers can step in make referrals and develop resources. Policy changes can be made to increase the number of assisted care facilities and To allow direct payment to long term assisted care facilities. Treatment of the underlying physical and/or mental medical condition/s a homeless person has is more effective than building and maintaining more and mor homeless shelters.
I agree, Connie.
As you know, most of these folks receive Medicaid. One of the problems they face is the lack of enough providers willing to participate with their Medicaid managed care plans, particularly the for-profit Ohana/Wellcare and UnitedHealthCare plans. Alohacare can also be difficult to work with.
The result is led access to care, fewer claims, fewer claims paid and more profit. Costs are shifted to state, local and private agencies. Sicker, higher utilizing members of these plans are more likely to encounter access problems compared to healthy members. Some of these “high utilized” go on to switch to another Quest plan out of frustration and necessity, often one of the non-profit plans with better provider networks (HMSAQuest, KaiserQuest). This burdens the non-profit plan with sicker members while the mismanaged plans benefit from a lower risk pool.
This is part of profitable business model for Ohana/Wellcare and UnitedHealthCare, and it is possible only because state officials with DHS-MedQuest for years have failed to properly enforce the Medicaid contacts.
“The result is LESS access to care, fewer claims,..”
What’s wrong with this picture? A homeless guy who has made consistently poor life choices is has his major medical bills fully subsidized and is now living in government subsidized housing.
But when a hard working muddled class family has a member come down with cancer or other grave disease, they’d have to pay the medical bills and often go into longterm debt.
What’s wrong with this picture ?
Isn’t America wonderful?……so many want to come if they can.
Rampant Mass-Immigration is the problem. The more crowded our country gets, the worse the ratrace is becoming, making it harder for sub-efficient-humans to live normally . So they give up and turn into subhumans, living more like pre-civilization creatures.
Your repeated dehumanizing comments are creepy.
Yes. Something is terribly wrong with the picture.
After taking drugs for 27 years finally at age 57 began to turn his life around. Seems more like after started having issues with his health problems. Probably health issue caused by abusing drugs. Now his health issues require expensive treatment paid by others. Typical story of the homeless.
Getting free medical care, free housing, and free food hardly qualifies as turning one’s life around. “Looking” for a job is a start, but “getting” a job actually might be the beginning of something real….
I thought Obamacare was supposed to stop this! Another lie.